Lol, okay I know the ladies mostly are going to laaaawwwv this. A dermatologist once told me that any hair or skin product with coconut oil does magic. Yes, we know coconuts are high in antioxidants especially vitamin E which protects the skin from oxidative damage and adds this infinite glow. Let’s see some other reasons why coconut oils are the best choice in keeping a healthy and marvelous skin:
1.) Recent research has shown that the use of coconut oil on the skin improved hydration and kept the skin surface lipids intact. It also stated that when it came to thick, scaly, fissured feet or rough leathery elbows and knees, coconut oil definitely beat regular moisturizer to the finish line.

2.) Coconut oil is an excellent moisturizer and with good anti-inflammatory properties (related to antioxidants such as polyphenols) keeps eczema in check. Dermatologists recommend using it right after your bathe, that way you lock in the moisture on your skin, leaving it soft, supple and lovely. Further, coconut oils’ content of medium chain fatty acids held decrease trans epidermal water loss, thereby reducing water loss in those with dry, sensitive skin, or atopical dermatitis.
3.) The combination of anti-inflammatory, antioxidant, antibacterial and hydrating properties make it truly unique. According to the Advanced Dermatology PC in Westchester, NYC, coconut oil is composed primarily of saturated fats and medium chain fatty acids which not only help to repair the skin barrier and trap water, thus hydrating the skin, they also reduce inflammation.
4.) In one study, coconut oil reduced protein loss in both damaged and undamaged hair when used before shampooing and as aa leave-in treatment. Coconut oil is able to penetrate the hair shaft due to its low molecular weight and affinity for proteins.

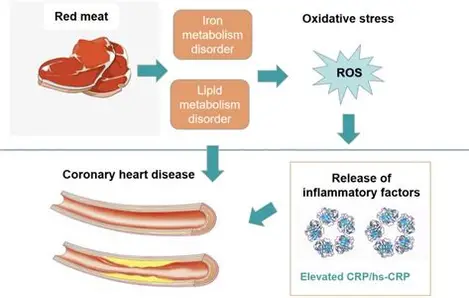
On another note, there seems to be emerging evidence that coconut oil may be healthy for the heart and body! This evidence suggests that its anti-inflammatory properties and MUFA content has been found to increase “good cholesterol” HDL, and that people who consumed extra virgin coconut oil reduced weight as well. However, this is not the main focus of this blog post. That would be addressed at a later post.
CAUTION:
Not everyone should apply it head to toe, such as those with very oily skin. For persons with acne-prone skin, it has been found to be comedogenic. However, the anti-inflammatory and anti-aging benefits of the polyphenols also make coconut oil part of a rejuvenating skin care regimen.
Of course, we know that anything that is good for the hair would be phenomenal for the skin and nails, as these are basically made up of keratin, which need to be nourished with vitamins and protein. So whether you are using this gift of nature for your cuticles, for your daily hair and skin health, you can be certain you are doing your looks a world of good with coconut oil. Who said skin care needed to be expensive?
Final Note: There are tons of real-life testimonials that say slathering the raw oil on hair and skin are a part of a daily beauty routine for them, I however recommend an enriched skin/hair cream. It guarantees smoother hair; more shine and not to mention crazy soft skin!