Definition
According to Wikipedia, “Vaginismus, sometimes called vaginism and genito-pelvic pain disorder, is a condition that affects a woman’s ability to engage in vaginal penetration, including sexual intercourse, manual penetration, insertion of tampons or menstrual cups, and the penetration involved in gynecological examinations (pap tests)”.
Types of Vaginismus:
Vaginismus can be experienced by women at any age or time in life. There are two major classifications:
* Primary vaginismus and
*Secondary vaginismus.
The medical community typically uses these terms to indicate the time of onset. These labels assist the professionals and researchers in diagnosis and classification. For the individual woman, the distinction between the two types tend to be of low significance. The good news is that both are highly treatable.
Primary Vaginismus:
Primary vaginismus usually refers to the experience of vaginismus with first-time intercourse attempts. Usually, primary vaginismus will be discovered when a woman attempts to have sex for the very first time. The spouse/partner is unable to achieve penetration and it is like he “bumps into a wall” where there should be the opening to the vagina, making entry impossible or extremely difficult. Primary vaginismus is a common cause of many sexless, unconsummated marriages. Some women with primary vaginismus will also experience problems with tampon insertion or having gynecological exams.
Primary vaginismus is often idiopathic.
Secondary Vaginismus:
Secondary vaginismus usually refers to the experience of developing vaginismus a little later in life, after a period of pain-free intercourse. Medical conditions such as yeast infections, cancer, trauma (such as rape) or thinning of the vaginal walls due to menopause can trigger the vaginismus condition. Vaginismus should be considered when a woman continues to experience ongoing sexual pain after her medical problem has been treated and healed. A woman’s ability to experience orgasms can also be affected as a sudden pain spasm may abruptly terminate the arousal buildup toward orgasm (we would all agree that this can be a nuisance). Some women with secondary vaginismus may also experience difficulty with gynecological exams or tampon insertion due to involuntary tightness.
Variations in the Classifications:
Note that these definitions can be a bit restrictive in some cases. For example, some women are able to tolerate years of uncomfortable but bearable intercourse with gradually increasing pain and discomfort that eventually becomes so pronounced that sex is no longer bearable. Women may also experience years of intermittent difficulty with entry or movement and have to constantly be on their guard to try to control and relax their pelvic area when it suddenly “acts up.”
Vaginismus has a wide range of manifestations, from impossible penetration, to intercourse with discomfort, pain or burning, all resulting from involuntary pelvic tightness.
Other Classifications:
Beyond the above basic classifications, physicians and specialists may use other medical terms referring to vaginismus such as:
Apareunia is a general term that refers to a condition where one is unable to have sexual intercourse. Vaginismus is one type of apareunia (if it is completely preventing penetrative intercourse).
Causes of Vaginismus
Some common triggers for Vaginismus include:
*Fear of pain associated with penetration, particularly the popular misconception of “breaking” the hymen upon the first attempt at penetration, or the idea that vaginal penetration will inevitably hurt the first time it occurs.
*Chronic pain conditions and harm-avoidance behaviour.
any physically invasive trauma (not necessarily involving or even near the genitals)
*Generalized anxiety
*Stress
*Negative emotional reaction towards sexual stimulation, e.g. disgust both at a deliberate level and also at a more implicit level.
*Strict conservative moral education, which also can elicit negative emotions.
Etiology:
The pain experienced during vaginismus is caused by the involuntary contraction of the pelvic floor muscles – specifically the pubococcygeus (PC) muscle group – leading to generalized muscle spasm and temporary cessation of breathing. Most times this is involuntary and psychological.
Treatment:
Vaginismus is highly treatable. Successful vaginismus treatment does not require drugs, surgery, hypnosis, nor any other complex invasive technique. It is mostly psychological in nature. Effective treatment approaches combine pelvic floor control exercises, insertion or dilation training, pain elimination techniques, transition steps, and exercises designed to help women identify, express and resolve any contributing emotional components.
Sex Therapy & Counseling:
Education typically involves learning about your anatomy and what happens during sexual arousal and intercourse. You’ll get information about the muscles involved in vaginismus too. This can help you understand how the parts of the body work and how your body is responding. Counseling may involve you alone or with your partner. Working with a counselor who specializes in sexual disorders may be helpful. Relaxation techniques and hypnosis may also promote relaxation and help you feel more comfortable with intercourse.
Vaginal Dilators:
Your doctor or professional may recommend learning to use vaginal dilators under the supervision of a professional.
Place the cone-shaped dilators in your vagina. The dilators will get progressively bigger. This helps the vaginal muscles stretch and become flexible. To increase intimacy, have your partner help you insert the dilators. After completing the course of treatment with a set of dilators, you and your partner can try to have intercourse again.
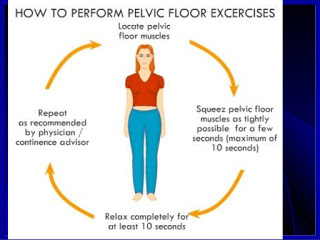
Kegel Exercises:
To perform Kegel exercises, repeatedly tighten and relax your pelvic floor muscles, which control your vagina, rectum, and bladder. You can locate these muscles when you’re urinating. After you begin to urinate, stop the stream. You’re using your pelvic floor muscles to do this. You may feel them tighten and move. These muscles move as a group, so they all contract and relax at the same time.
Practicing these exercises helps you control when your muscles contract and relax. Follow these steps:
- Empty your bladder.
- Contract your pelvic floor muscles, and count to 10.
- Relax your muscles, and count to 10.
- Repeat this cycle 10 times, three times a day.
- To successfully strengthen your pelvic floor muscles, don’t engage the muscles of your abdomen, buttocks, or thighs when doing these exercises.
After a few days, insert one finger, up to about the first knuckle joint, inside the vagina while doing the exercises. It’s a good idea to clip your fingernails first and use a lubricating jelly. Or do the exercises in a bathtub, where water is a natural lubricant. Start with one finger and work your way up to three. You’ll feel the vagina’s muscles contracting around your finger, and you can always take your finger out if you’re not comfortable.
This approach is called progressive desensitization and the idea is to get comfortable with insertion.
Sources: