DIABETES: WHAT’S NEW? 2
Yesterday we treated most of the points under this article. Now we are just going to round up. Enjoy!
Fructose:
People with diabetes should limit or avoid intake of sugar-sweetened beverages (SSBs) (from any caloric sweetener including high-fructose corn syrup and sucrose) to reduce risk for weight gain and worsening of cardiometabolic risk profile.
Fructose is a monosaccharide found naturally in fruits. It is also a component of added sugars found in sweetened beverages and processed snacks. The term “free fructose” refers to fructose that is naturally occurring in foods such as fruit and does not include the fructose that is found in the form of the disaccharide sucrose, nor does it include the fructose in high-fructose corn syrup.
Non-nutritive Sweeteners and Hypocaloric Sweeteners:
Use of nonnutritive sweeteners (NNSs) has the potential to reduce overall calorie and carbohydrate intake if substituted for caloric sweeteners without compensation by intake of additional calories from other food sources.
The U.S. Food and Drug Administration has reviewed several types of hypo-caloric sweeteners (e.g., NNSs and sugar alcohols) for safety and approved them for consumption by the general public, including people with diabetes. Research supports that NNSs do not produce a glycemic effect; however, foods containing NNSs may affect glycemia based on other ingredients in the product. An American Heart Association and ADA scientific statement on NNS consumption concludes that there is not enough evidence to determine whether NNS use actually leads to reduction in body weight or reduction in cardiometabolic risk factors. These conclusions are consistent with a systematic review of hypocaloric sweeteners (including sugar alcohols) that found little evidence that the use of NNSs lead to reductions in body weight. If NNSs are used to replace caloric sweeteners, without caloric compensation, then NNSs may be useful in reducing caloric and carbohydrate intake, although further research is needed to confirm these results.
Protein:
For people with diabetes and no evidence of diabetic kidney disease, evidence is inconclusive to recommend an ideal amount of protein intake for optimizing glycemic control or improving one or more CVD risk measures; therefore, goals should be individualized.
For people with diabetes and diabetic kidney disease (either micro- or macroalbuminuria), reducing the amount of dietary protein below the usual intake is not recommended because it does not alter glycemic measures, cardiovascular risk measures, or the course of glomerular filtration rate (GFR) decline.
In individuals with type 2 diabetes, ingested protein appears to increase insulin response without increasing plasma glucose concentrations. Therefore, carbohydrate sources high in protein should not be used to treat or prevent hypoglycemia.
Total Fat:
Evidence is inconclusive for an ideal amount of total fat intake for people with diabetes; therefore, goals should be individualized.Fat quality appears to be far more important than quantity.
Fatty acids are categorized as being saturated or unsaturated (monounsaturated or polyunsaturated).Transfatty acids may be unsaturated, but they are structurally different and have negative health effects. The type of fatty acids consumed is more important than total fat in the diet in terms of supporting metabolic goals and influencing the risk of CVD; thus more attention should be given to the type of fat intake when individualizing goals. Individuals with diabetes should be encouraged to moderate their fat intakes to be consistent with their goals to lose or maintain weight.
Recent studies of fat intake and diabetes incidence support the notion that eating the right kind of fats is beneficial to health. This goes against years of advocacy of a low-fat/high-carbohydrate diet. “When people started eating less fat, they compensated by eating more refined carbohydrates, which stimulate insulin secretion and increase fat deposition. A major problem with the American diet is too much refined grains and added sugar, which are associated with the rise in obesity and type 2 diabetes,” Dr. Hamdy says.
(adsbygoogle = window.adsbygoogle || []).push({});
Current evidence shows that some fats, such as those from red and processed meats, are associated with higher cardiovascular risk while other fats such as those from vegetable oils and nuts are associated with lower risk. The Joslin nutritional guidelines for diabetes recommend a diet with relatively high amounts of healthy fats and protein but moderately low amounts of carbohydrates.
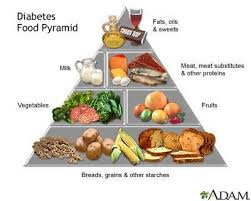
Making the glycemic index easy
The glycemic index (GI) tells you how quickly a food turns into sugar in your system. Glycemic load, a newer term, looks at both the glycemic index and the amount of carbohydrate in a food, giving you a more accurate idea of how a food may affect your blood sugar level. High GI foods spike your blood sugar rapidly, while low GI foods have the least effect.
You can find glycemic index and glycemic load tables online, but you don’t have to rely on food charts in order to make smart choices. Australian chef Michael Moore has come up with an easier way to regulate the carbs you eat. He classifies foods into three broad categories: fire, water, and coal. The harder your body needs to work to break food down, the better.
A. Fire foods:
They have a high GI, and are low in fiber and protein. They include “white foods” (white rice, white pasta, white bread, potatoes, most baked goods), sweets, chips, and many processed foods. They should be limited in your diet.
B. Water foods:
These are free foods—meaning you can eat as many as you like. They include all vegetables and most types of fruit (fruit juice, dried fruit, and canned fruit packed in syrup spike blood sugar quickly and are not considered water foods).
C. Coal foods:
These have a low GI and are high in fiber and protein. They include nuts and seeds, lean meats, seafood, whole grains, and beans. They also include “white food” replacements such as brown rice, whole-wheat bread, and whole-wheat pasta.
Controlling weight with the glycemic index
Researchers believe that the key to weight control lies in reducing the amount of refined carbohydrates (“white” or “fire” foods) in your diet. Instead, focus on low GI or “coal” foods which keep you feeling fuller much longer. Low-glycemic foods take longer to digest so sugar is absorbed more slowly into the bloodstream. As a result you’re less likely to experience a spike in your blood sugar level, you’ll remain sated for longer, and are less likely to overeat.
Avoid processed foods like baked goods, sugary desserts, and packaged cereal and opt instead for steel cut oats, beans, fat-free low-sugar yogurt, dark green leafy vegetables, and whole grains.
Eat whole fresh fruit instead of fruit juice—squeezing fruit releases more sugar so a whole orange has a lower GI than a glass of juice.
Full adherence to the guidelines of this article should afford a diabetic a full, happy life. Stay Healthy Please!
previous article
DIABETES: WHATS NEW?
next article
THE DASH TOWARDS GOOD HEALTH
The author Prince
Hi, I’m Prince.. a registered Dietitian, an avid reader and a passionate writer. I hope you enjoy my articles as much as I enjoy writing them